
CALCIFYING TENDINITIS OF THE SHOULDER
Calcifying tendinitis of the shoulder is a painful acute or chronic disorder characterized by calcifications in rotator cuff tendons.
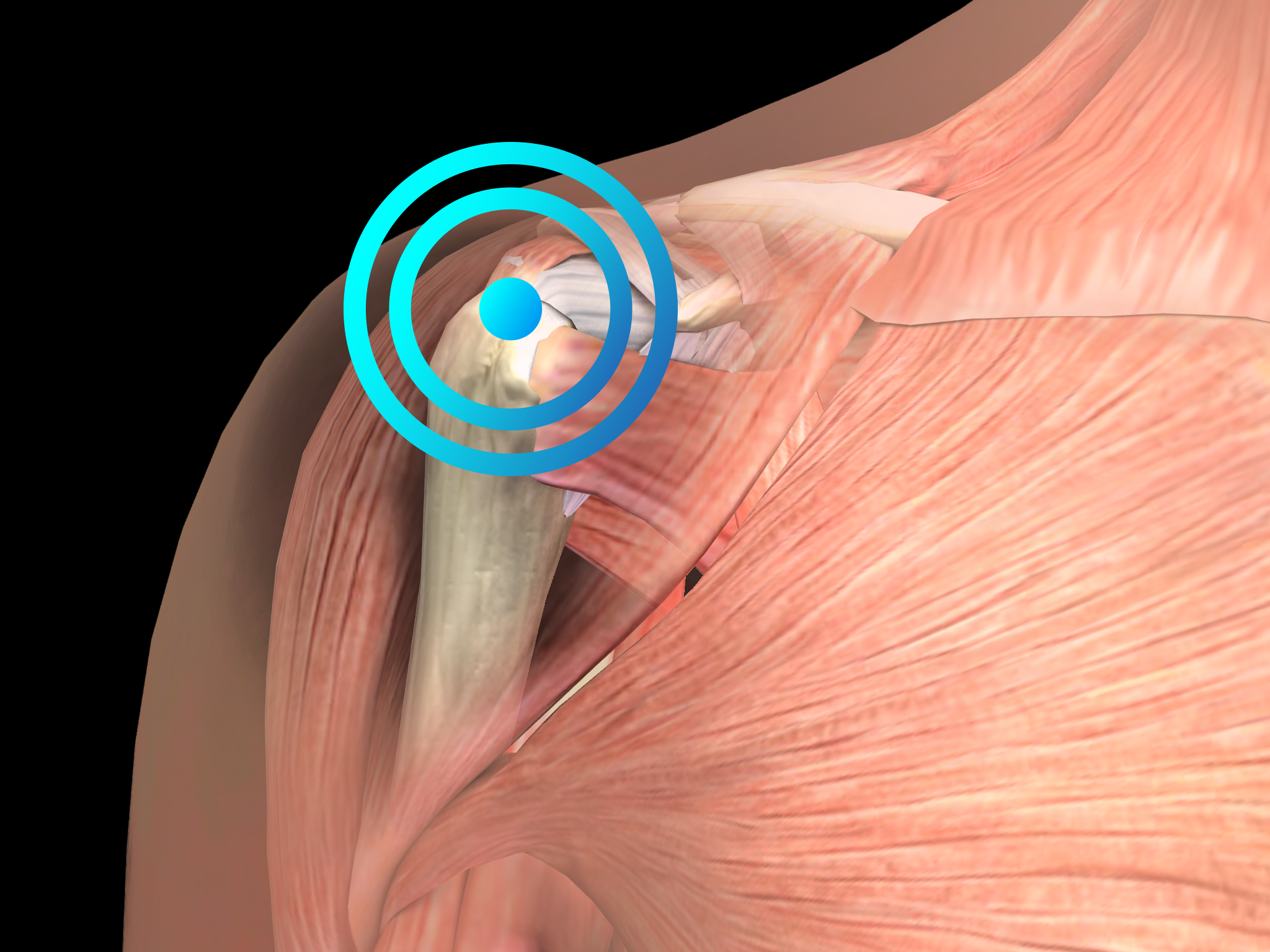
Pathology
The main clinical symptom is shoulder pain, often aggravated by lying on the shoulder or elevation of the arm above the shoulder level. The patient may be awoken from sleep by the pain. Other complaints may be weakness, stiffness, snapping, or catching of the shoulder. Diagnosis is based on the clinical features of the disease and on imagery. The calcifications occur most commonly in the supraspinatus tendon (51%–90%) and least commonly in the subscapularis tendon (3%).
The etiology is largely unknown. It has been hypothesized that the condition may be related to hypovascularity-induced fibrosis and necrosis within the tendon with subsequent degeneration. The characteristics of an existing, symptomless calcific deposit may be changed by minor traumatic episodes, leading to acute symptoms. The condition may also be related to mechanical irritation by deposits when the arm is abducted and deposits impinge on the acromion.
The disease usually presents in four stages:
- Precalcific stage (usually without symptoms), involving fibrocartilaginous metaplasia within the tendon;
- Formative phase (with or without pain), with calcific deposits formed in the fibrocartilaginous matrix;
- Resorptive phase (massive pain), with deposits disappearing by cell-mediated resorption (inflammatory response); and
- Final stage (with or without pain), involving healing and rotator cuff repair. Notably, this cycle can be blocked at any one stage in chronic calcifying tendinitis.
The incidence is approximately 3% in the healthy population and approximately 7% in those with shoulder pain. The predominant age is 30 to 50 years. Women are two times more affected than men.
The initial treatment should be conservative including rest, physiotherapy, and nonsteroidal anti-inflammatory drugs. In later stages, radial shock wave therapy (RSWT) should be considered (not in the resorptive phase), or subacromial infiltration with corticosteroids. Surgery should be considered for recalcitrant cases of calcifying tendinitis of the shoulder.
In later stages, radial shock wave therapy should be considered for calcifying tendinitis of the shoulder.
Side effects of Radial Shock Wave Therapy (RSWT) using the Swiss DolorClast®.
When performed properly, RSWT with the Swiss DolorClast® has only minimal risks. Typical device-related non-serious adverse events are:
- Pain and discomfort during and after treatment (anaesthesia is not necessary)
Reddening of the skin - Petechia
- Swelling and numbness of the skin over the treatment area
These device-related non-serious adverse events usually disappear within 36h after the treatment.
Treatment Procedure
Clinical Proof
Radial shock wave therapy of rotator cuff tendinosis calcarea - A prospective study
Magosch P, Lichtenberg S, Habermeyer P
Z Orthop Ihre Grenzgeb 2003; 141 : 629-636
(Study in German)
Effectiveness of extracorporeal shock wave therapy in calcifying tendinitis of the shoulder
Gremion G, Augros R, Gobelet C, et al.
2000
(Study in French)
Recommended Settings
| Recommended Settings | Treatment |
| Number of treatment sessions | 3 to 5 |
| Interval between two sessions | 1 week |
| Air pressure Evo Blue® | 2 to 4 bar |
| Air pressure Power+ | 1.5 to 3 bar |
| Impulses | 2000 on the painful spot |
| Frequency | 8Hz to 12Hz |
| Applicator | 15mm |
| Skin pressure | Heavy |
Contraindications
The following contraindications of RSWT using the Swiss DolorClast® must be considered:
- Treatment over air-filled tissue (lung, gut)
- Treatment of pre-ruptured tendons
- Treatment of pregnant women
- Treatment of patients under the age of 18 years (except for Osgood-Schlatter disease and muscular dysfunction in children with spastic movement disorders)
- Treatment of patients with blood-clotting disorders (including local thrombosis)
- Treatment of patients treated with oral anticoagulants
- Treatment of tissue with local tumors or local bacterial and/or viral infections
- Treatment of patients treated with cortisone
Some indications may not be approved in the United States of America, under regulation by the US FDA. Please refer to the respective Instructions for Use.
